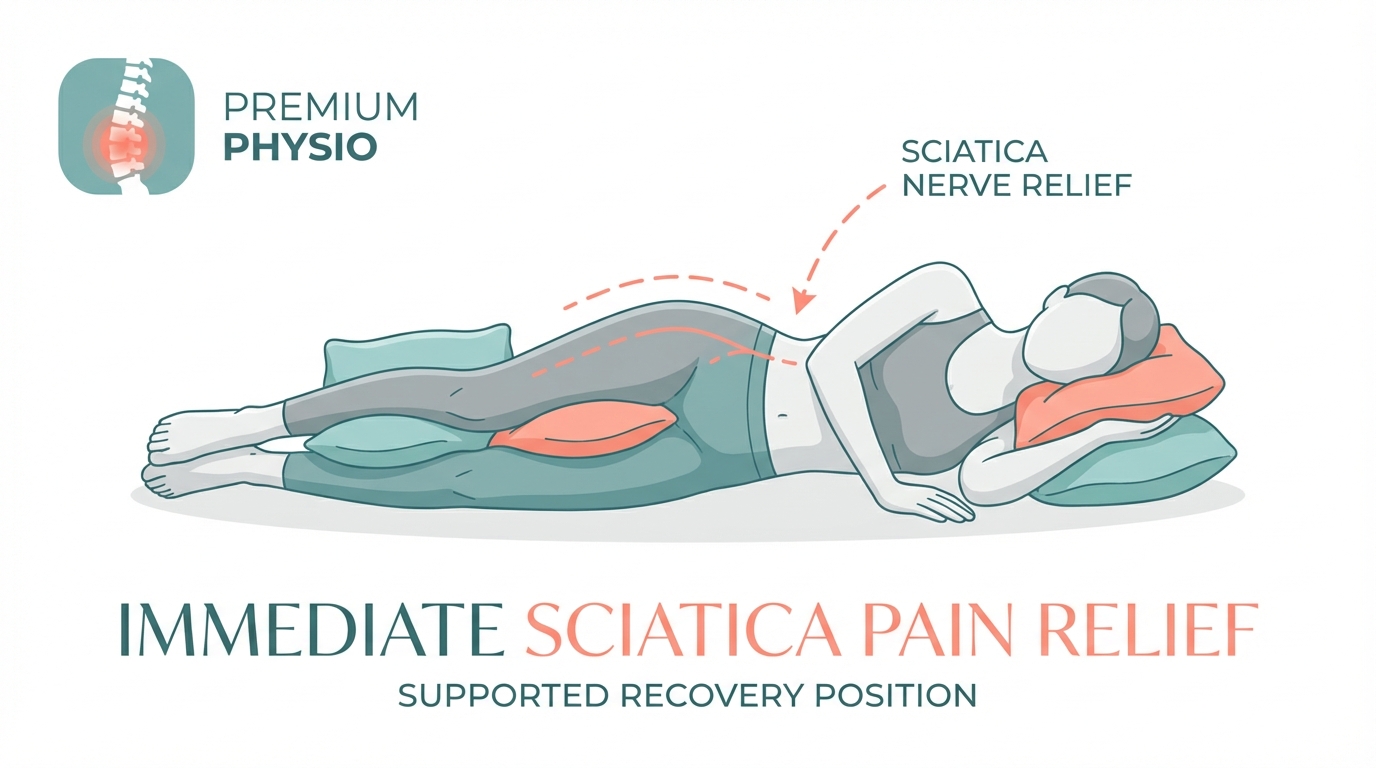
Sciatica recovery
Sciatica Recovery Guide
Evidence-based exercises and guided recovery programs for sciatic nerve pain.
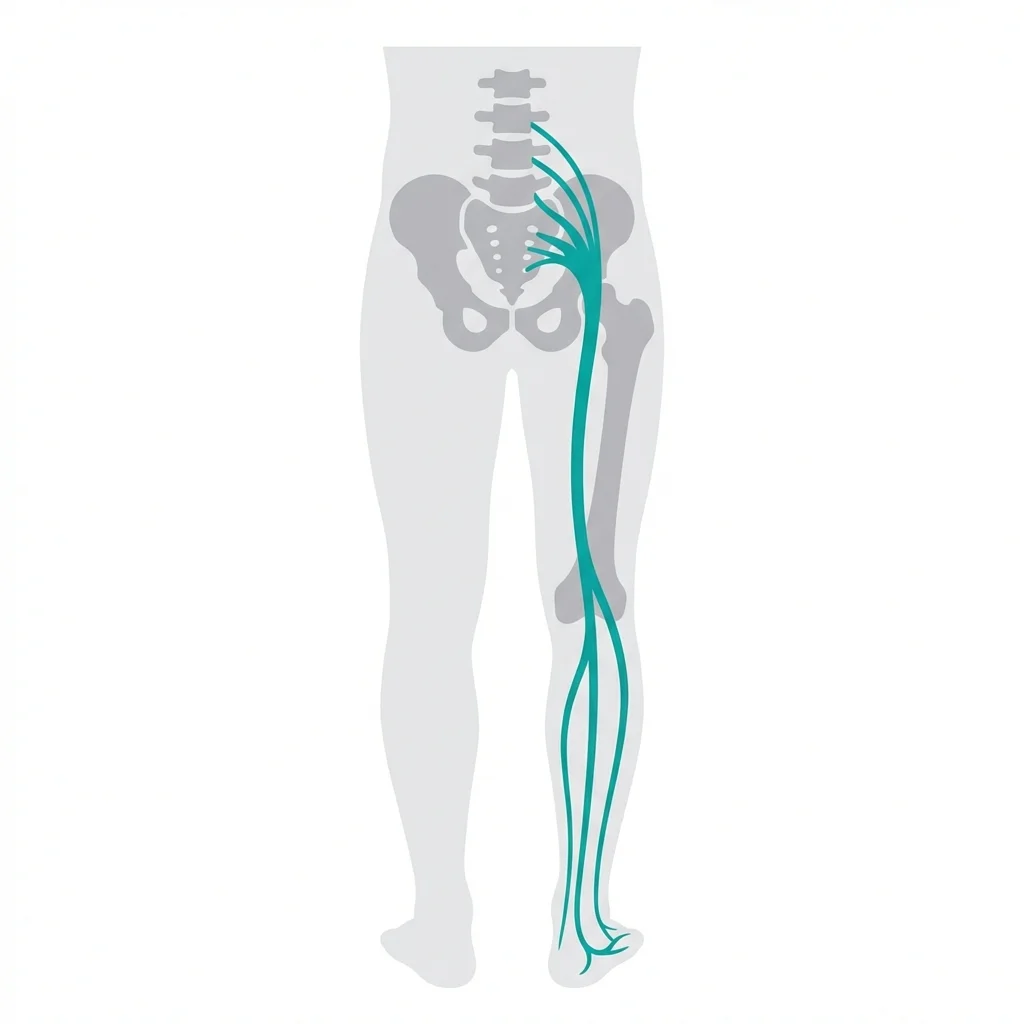
What is sciatica?
Sciatica is pain that radiates along the path of the sciatic nerve — from your lower back through your hips and down each leg. It’s usually caused by a herniated disc, spinal stenosis, or other conditions that compress or irritate the nerve.
Pain can range from mild to severe and may be accompanied by numbness, tingling, or weakness. While sciatica can be debilitating, most cases respond well to structured, evidence-based rehabilitation.
Common symptoms of sciatica
Sciatica symptoms vary in intensity and location. Recognizing them early helps guide the right recovery approach.
Leg pain
Sharp or burning pain that radiates from the lower back down the leg, often following the sciatic nerve path.
Tingling
Pins-and-needles sensation in the leg, foot, or toes caused by nerve irritation.
Numbness
Reduced sensation or feeling in parts of the leg or foot along the sciatic nerve distribution.
Pain while sitting
Increased discomfort when sitting for prolonged periods, especially on hard surfaces.
Lower back pain
Dull ache or sharp pain in the lumbar region, often at the origin of nerve compression.
Foot weakness
Difficulty lifting the foot or toes, which can affect walking and balance.
Common causes of sciatica
Understanding the underlying cause helps determine the most effective recovery strategy.
Herniated disc
The most common cause. A disc in the lower spine bulges or ruptures, pressing on the sciatic nerve root.
Spinal stenosis
Narrowing of the spinal canal that puts pressure on the nerves, including the sciatic nerve.
Piriformis syndrome
The piriformis muscle in the buttock spasms or tightens, irritating the sciatic nerve beneath it.
Degenerative disc disease
Age-related wear on spinal discs can lead to nerve compression and sciatica symptoms.
Why guided recovery matters
Generic advice doesn’t account for where you are in recovery. Guided programs adapt to your phase and help you progress safely.
Evidence-based exercises
Every exercise is grounded in physiotherapy research and clinical best practices for sciatica recovery.
Adaptive recovery phases
Programs that adjust to your current pain level and progress, from acute relief to full recovery.
Safe progression
Clear guidance on when to advance, hold, or step back — so you never push too hard or too fast.
How recovery works
Our recovery programs follow a progressive structure designed to take you from pain relief to long-term maintenance.
Pain relief
Gentle movements and positions that reduce acute pain and centralize symptoms when possible.
Nerve mobility
Exercises that encourage the nerve to glide freely and reduce sensitivity over time.
Core stability
Building strength to support the spine and reduce the risk of recurrence.
Maintenance
Ongoing routines to keep you pain-free and prevent future flare-ups.
Get early access to Sciatica Relief
Join the waitlist for our first guided sciatica recovery program — evidence-based exercises, structured phases, and clear progression.
Related sciatica articles
Frequently asked questions
Ready to start your recovery?
Join hundreds of others using evidence-based guided rehabilitation for sciatica recovery.
Join the early access list